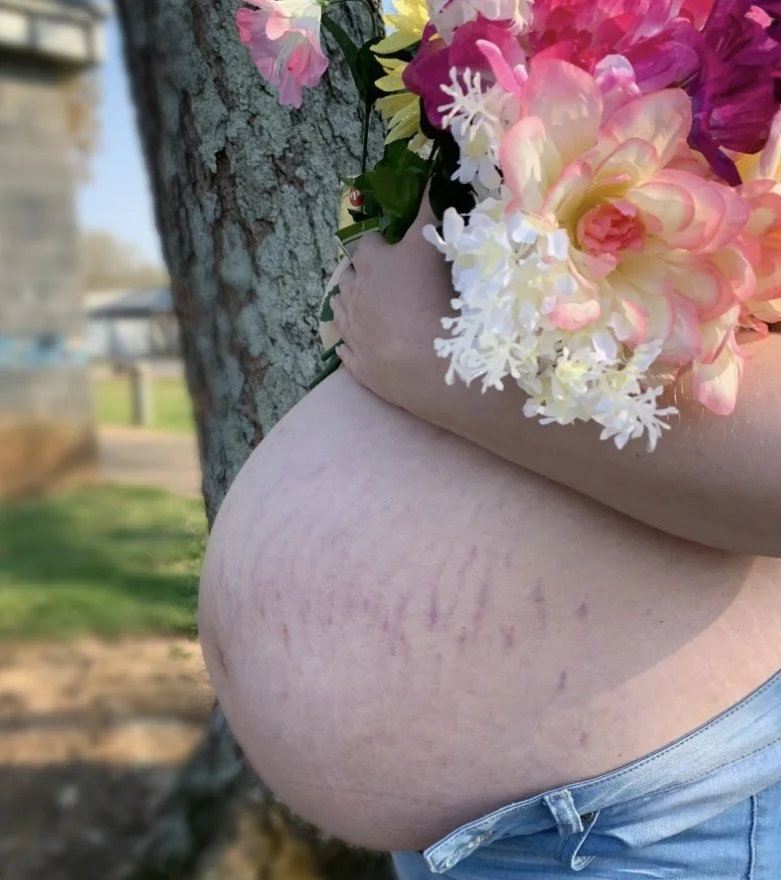
This Is Our Firstborn Daughter Alara’s Story
My daughter didn’t stop growing.
Her placenta did.
And no one measured it.
This is the story of a love that began before birth and a loss that changed everything—one that could have been prevented.
We share it to honor her life and in hopes of raising awareness about preventable stillbirth.
A baby who fought.
A system that did not.
Please read gently.
⸻
Alara: A Story of Love, Warning Signs, and Silence
I carried you, and I loved you the moment I found out we created you. But when I heard your heartbeat, that love became fierce. Different. It became war when it came to you.
⸻
Chapter One: Before the World Knew
We didn’t insist on getting pregnant—it just happened. And we are glad it did.
On September 3, 2024, something quiet shifted inside me—so subtle that no one noticed it but my body. I didn’t know it yet, but you had already begun. Love had already taken root.
By October 9, 2024 my body made it undeniable. The nausea. The vomiting. The missed period. My body whispered before the test ever screamed the truth.
When I told your daddy, the look on his face said everything: shock, joy, disbelief, and love colliding all at once.
From that moment on, you were no longer just my secret.
You were our miracle.
We went straight to the health department to find out I was 7 weeks along.
I felt awe.
I felt chosen.
As if the universe had placed something sacred inside me and whispered, ‘Protect this.’
Before the world ever met you, you were already deeply loved and wanted. You were cherished by your grandparents on both sides—who loved you and spoke of you with pride and excitement. You were wanted, prayed over, and celebrated. Your family dreamed of holding you, watching you grow, and loving you for a lifetime.
Your cousins, aunts, and uncles were ready to know you and to grow up alongside you. You were never alone. You were surrounded by love from the very beginning, and you continue to be loved and celebrated by your family every single day.
We talked about you—about names, about who you might look like, about the future. We planned everything. We changed our lives.
On November 4, 2024, at eleven weeks, I heard your heartbeat for the first time. Fast. Strong. Steady. I cried happy tears.
It is still my favorite sound.
I was eager for every ultrasound, every appointment, every chance to see you, hear you, and watch you grow.
I had my first Thanksgiving feeding you while you were in my tummy. Then Christmas. Then the New Year 2025—the year you were expected to arrive and come home with us.
⸻
Chapter Two: Becoming Your Safe Place
I did everything right. I attended every appointment. I asked extra questions. I learned extra knowledge. I downloaded all the apps. I knew how you were developing. I knew when your eyes opened. I knew when it was time for you to start hearing in my womb.
Your family would sing to you and use a at-home Doppler to hear your precious heart. I purchased this Doppler because I wanted to know you were okay at all times.
I kept up with you. I was waiting for you.
Time moved so fast and so slow at the same time. I hit eight months and felt so relieved knowing my baby would be in my arms within’ two months or less.
I bought you things. It felt like you were here all along—like you belonged here all along. We were so proud. We still are proud of you. My belly was full of love, and our life was brighter.
I can still feel your kicks today. I was one of those moms who tracked every appointment with notes. I was already preparing to find you a pediatrician and schedule your doctor visits after birth. I had everything ready to a T for you and for our life together.
I didn’t have too much caffeine. I ate healthy. I read all the books. I prepared myself. I did everything to get ready for motherhood—to take care of my newborn. I made sure my bath water wasn’t too hot. I was always cautious. I laid on my side.
You used to kick your daddy when I laid on my side holding him with his back to my belly—like, no, this is my space, get away from mommy. So cute. Full of humor. Sassy little girl.
By ten weeks, the sickness disappeared.
By twelve weeks, my body began leaking breast milk—already preparing to nourish you.
At thirteen weeks, I was diagnosed with gestational diabetes.
I failed the one-hour glucose test. Then the three-hour test.
I changed everything immediately—low carb, no sugar. I checked my blood sugar four times a day: fasting, then two hours after breakfast, lunch, and dinner. Every Wednesday, I sent my numbers to my specialist. They were controlled.
Because of this diagnosis, my pregnancy was labeled high-risk.
I believed that meant closer attention.
More protection.
Your daddy learned everything alongside me—what I could eat, what I couldn’t, how to help when I felt overwhelmed. He celebrated my good numbers and reassured me when I worried.
On November 14, 2024, a blood test revealed your gender.
You were a girl.
My girl.
Our girl.
I knew I was going to have a mini me—a mini us. I dreamed of playing dress-up, doing your hair, and sharing all the girly things with you.
Your daddy dreamed of you playing sports. Your daddy smiled differently after that—softer, prouder, more protective.
At sixteen weeks, my belly began to show.
At seventeen weeks, I felt you constantly—not just at night, but all day, every day.
At twenty-one weeks, I could see your movements beneath my skin. We watched in awe, already knowing our baby was full of personality.
At twenty weeks and five days, during a long anatomy scan, the ultrasound technician laughed and called you “spicy.” You kicked and rolled nonstop for nearly thirty minutes. You weighed fourteen ounces. Your daddy called you his little athlete.
You earned an A+.
Everything felt perfect.
What no one was watching closely enough was the organ keeping you alive.
⸻
Chapter Three: Signs Without Answers
On February 18, 2025, at twenty-four weeks, doctors identified a concern.
They found you were swelling—your abdomen and legs. You weighed two pounds, three ounces.
All tests came back negative.
They didn’t know why.
No one explained what it meant.
They said we would find out after birth.
At twenty-five weeks and five days, they told me nothing had changed. Your swelling “looked the same.” Your heartbeat was good. There was “no fluid” retained in the swelling.
That same day, I took a picture of your ultrasound with my phone. I didn’t know why—just instinct.
Looking back now, the image clearly shows swelling in your eye.
The same eye that was visibly swollen after birth.
For eight weeks, you stayed swollen. They first found it at twenty-four weeks… and by the time you passed, you were nearly thirty-two weeks along.
Eight long weeks of holding on. Of loving you through every moment.
Eight weeks of the doctors repeatedly telling me “it’s just in the abdomen and legs.”
They kept telling me nothing had changed.
No one explained that prolonged swelling can be a sign of fetal stress or compensation from reduced oxygen or blood flow.
At twenty-seven weeks, you weighed three pounds, nine ounces.
You were strong.
⸻
Chapter Four: Missed Warnings
At twenty-eight weeks pregnant, on March 13, 2025, around 9:00 PM, I twisted my ankle and I fell outside while walking to my car. Almost immediately, the contractions started.
We went to the hospital to be safe.
They admitted me overnight because the contractions were coming back-to-back, and at first, they believed my water had broken. A test even showed what looked like amniotic fluid under the microscope. Later, they changed course and told me it hadn’t actually broken.
They tried to reach my OB and high-risk care team—but no one answered.
Meanwhile, you were incredibly active on the monitors. The nurses even joked, “Does she ever sleep?”
But you weren’t just active.
You were fighting.
The next morning, March 14 at 10:00 AM, they discharged me. They said the contractions were just a result of the fall.
So we trusted them.
⸻
Chapter Five: The Night Everything Shifted
On March 31, 2025, at thirty weeks and four days, I saw my OBGYN for a routine appointment.
During that visit, she told me she had noticed something on my bloodwork that she didn’t fully understand. She said she was “a little concerned, but not too terribly.”
She advised me to follow up with my high-risk doctor at my next scheduled appointment on April 8, 2025.
No additional testing was ordered.
No urgency was communicated.
We were sent home to wait.
At that point, my pregnancy had already shown weeks of unexplained swelling, repeated abnormal ultrasound findings, and ongoing concerns that had never been clearly explained or resolved.
Still, we trusted that waiting was safe.
Around this time, I was told that baby girl would turn into position for birth in a couple of weeks.
⸻
Chapter Six: Silence
On April 6, 2025—two days before the next appointment my OBGYN told me to wait for—I felt no movement. It was sudden and out of nowhere.
I went to the hospital.
By the time I arrived, my body had already begun to dilate on its own—one centimeter.
They tried to find your heartbeat but struggled. They had me turn onto my side, hoping for a clearer reading. At one point, they briefly thought they had found it—but it was mine. I wish it had been yours.
They looked at me, gently placed a hand over mine, and said, “I’m so sorry. There is no heartbeat. There is no blood flow to the brain.”
I won’t go into what came after.
In that single moment, everything changed. Our lives were never the same again.
This is a loss we will carry for the rest of our lives—a deep, aching absence that will stay with us until the day we meet you again.
Your entire family came, surrounding us with love, standing beside us in the middle of the unimaginable.
⸻
Chapter Seven: The Day You Entered the World and Returned to Heaven
On April 7, 2025, at 31 weeks and 6 days, I gave birth to you—a day before I was supposed to be at that high-risk appointment for more “tests.”
You were born sleeping.
You weighed 5 pounds, 3 ounces.
You measured 19.5 inches.
You had a full head of black hair.Mommy’s lips and lip shape.Probably my eyes too—but I never got to see your eyes open.A mixture of mine and daddy’s chin. Daddy’s nose, eyelids, and hair color.
You were perfect.
Still.
Stillborn.
Still our baby.
Still loved.
Mommy and Daddy were sent home holding a stuffed teddy bear instead of our whole world—our daughter.
The human we created… the baby I carried… the girl we bonded with for eight months… the one we shared everything with… the one we had everything ready for… the child who changed our lives forever… the tiny girl I had my hospital bag packed for.
We never imagined a life without you, and it still feels unbearable.
April 7 will always belong to you, our little Aries.
We should be watching you grow, but those moments now live in our hearts.
You are our first, and you will always be at the center of our family.
⸻
Chapter Eight: The Organ That Sustained You
The placenta is the only organ created solely to sustain another life. It acts as a baby’s lungs, kidneys, liver, and digestive system. A baby can only grow as well as the placenta allows.
Early in pregnancy, the uterus is meant to transform its blood vessels—called spiral arteries—so they widen and allow enough blood to reach the placenta.
In my pregnancy, that transformation never fully happened. My spiral arteries did not widen.
This caused placental development problems from the very beginning. Blood flow and oxygen were restricted early on. The placenta never grew to the size it should have.
No one measured it.No one told us it should be measured.
A fetal autopsy showed she was perfectly normal, and her cause of death was listed as unknown.
In June, I came across another mother online—“Weylen’s mama”—sharing her stillbirth story. Like mine, every test had returned negative. She said everyone told her to contact Dr. Harvey Kliman.
Dr. Kliman is a research scientist at Yale University School of Medicine and Director of the Reproductive and Placental Research Unit. He has examined placental tissue from over 2,300 stillborn babies and can identify a likely cause in approximately 90% of cases.
I reached out to him in early July 2025. He responded quickly.
He reviewed my entire pregnancy—medical records, appointment notes, ultrasounds, pathology, autopsy results, photos of Alara after birth—and examined my actual placenta and umbilical cord.
Later, we learned that a placental weight of 283 grams was far too small to keep up with her growth.
Her placenta weighed 283 grams—not even a pound. Far too small for her size and gestational age.
Our baby continued to grow strong, but the placenta—the organ that delivers oxygen and nutrients—was underdeveloped and could not meet her increasing needs.
There was no infection.
No genetic abnormality.
No chromosomal issue.
Oxygen delivery became inadequate.
For a time, she was receiving just enough support to survive. There was no classic fetal growth restriction.
This is why placental insufficiency is often missed when the placenta is not measured.
A small placenta cannot compensate forever.
Babies can tolerate this condition—until suddenly, they cannot.
Even with a small placenta, a baby may continue to grow normally, until all of a sudden, they don’t.
Placental insufficiency can lead to:
• Chronic fetal hypoxia (low oxygen)
• Swelling (edema)
• Sudden fetal demise without warning
This directly aligns with what we were told about swelling and ongoing ultrasound concerns earlier in pregnancy.
We trusted the system.
We believed high-risk meant someone was watching closely.
They were not.
What I didn’t know then—but understand now—is that placental size matters just as much as fetal growth.
The autopsy confirmed swelling in different parts of your body—especially your eye—matching what ultrasounds had shown for weeks.
My baby survived as long as she did because she is strong. She fought until the end.
“Behind every healthy baby is a healthy placenta,” Dr. Kliman told me.
“The placenta is like the roots of a tree.”
Placental measurement matters.
Umbilical artery Dopplers matter.
Additional ultrasound measurements can save lives.
Now I speak so others can.
⸻
Chapter Nine: Why This Was Preventable
For eight weeks, Alara showed visible, documented signs of distress.
She was swelling.
Ultrasounds showed it.
Doctors acknowledged it.
Lots of things were brushed off, including a blood test and I got sent home with concerns instead.
They said they didn’t know why.
They said we would find out after birth.
The placenta was never measured.
Advanced monitoring was not escalated.
Early delivery was not offered.
I was not offered advanced ultrasounds.
A baby should not swell for eight weeks without action.NICUs exist for this exact reason. At her size and strength, early delivery could have saved her life.
Instead, she remained attached to a failing placenta.
Alara did not have to pass away.
Throughout my pregnancy, every lab result—blood and urine—showed that my immune system was highly revved up and my body was under significant stress! I have the medical records to prove it.
And yet, no one ever made me aware that anything was wrong.
No mother should be told everything is okay when it isn’t.No one should have concerns overlooked instead of acknowledged and talked through.
⸻
Chapter Ten: Everything We Lived
I lived every part of pregnancy.
The maternity clothes.
The maternity pictures.
The memories.
The belly creams.
The packed hospital bag.
The nursery—the theme: fairies.
The baby shower.
The gender reveal—December, Christmas-themed, gingerbread-themed.
The clothes washed and folded.
We had your baby shower one week before your passing, at the end of March. Fairy-themed everything—butterflies, mushrooms, a fairy world of pink and purple glitter. Lily pads.
I chose this theme because your name, Alara, means water fairy.
You gave me my title of mother.
You were my first pregnancy.
My first birth.
My first child.
Nothing and nobody will ever replace you.
Today, we are changed—but still standing.
We hold space for other families. We will carry this forever.
⸻
Chapter Eleven: Please Save a Life
My family isn’t the only family that experienced a stillbirth in 2025.
Placental insufficiency is detectable before loss. Estimated placental volume (EPV) and routine placental measurements during ultrasound can identify placentas early—allowing for increased monitoring or timely intervention.
My daughter’s life mattered. Her placenta told a story—but it was only heard after she was gone.
Measuring the placenta could have changed the outcome.
This is why placental measurements must become a standard part of prenatal care—not an afterthought discovered in pathology reports.
Help support Measure the Placenta’s mission to make placental measurements part of standard prenatal care.
Share your story on social media. Tag @measuretheplacenta and/or submit at measuretheplacenta.org/stories.
Volunteer to help Measure the Placenta spread awareness about preventable stillbirth and placental health.
Talk to your OB, MFM, or sonographer about measuring the placenta.
Measure the placenta.
⸻
We carry you in every breath, every step, and every tomorrow.
Loved for a lifetime. Missed beyond words.
Say her name today and always — Alara
In Loving Memory
Alara Nikole Sand
Born sleeping April 7, 2025
31 weeks, 6 days
5 lbs 3 oz • 19.5 inches
My firstborn.
My warrior.
My forever.
⸻
Written by:
Alexis Womble
January 2026
© 2026 Alexis Womble & Aaron Sand. All rights reserved.